Historical Evolution of Doctor-Patient Dynamics
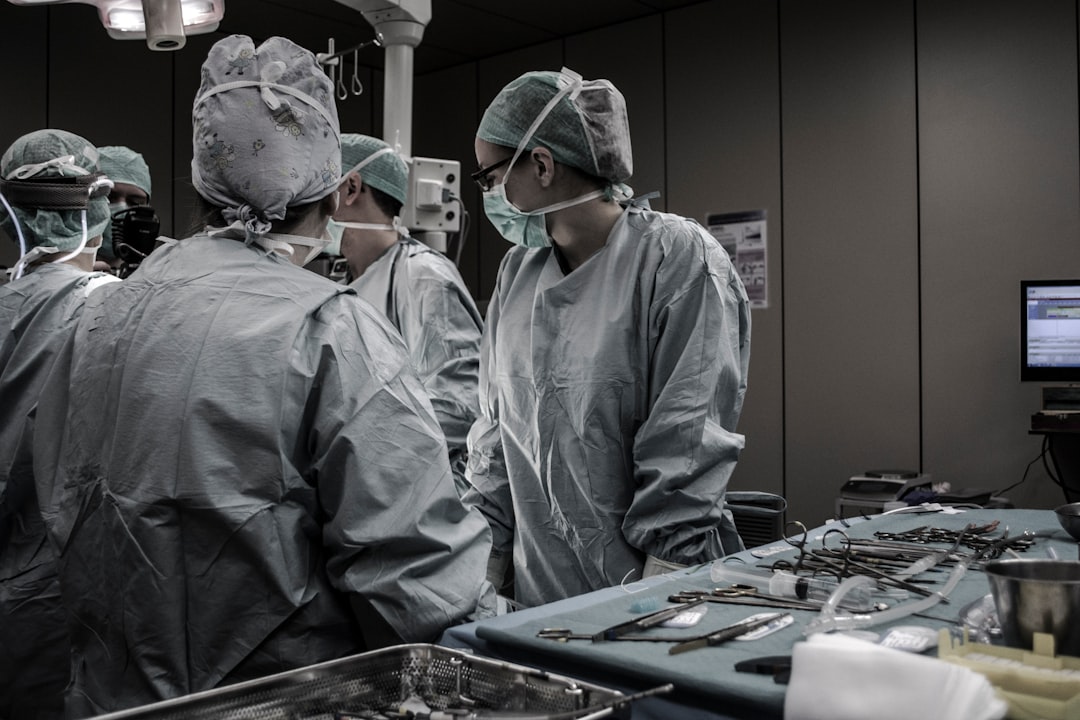
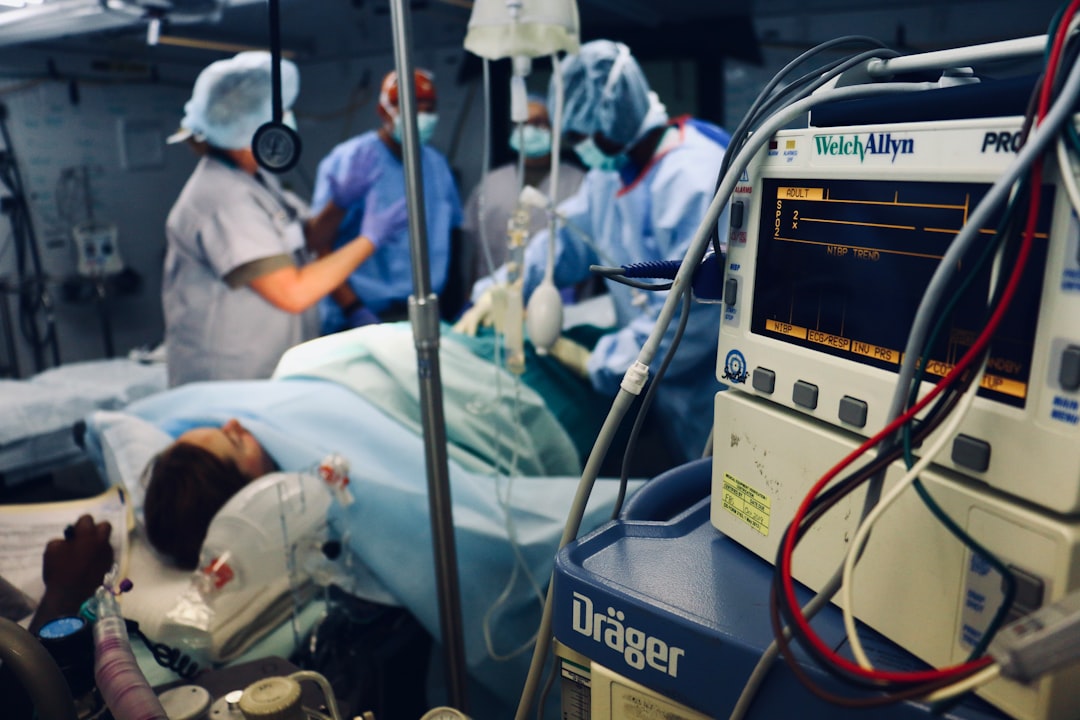
The historical evolution of doctor-patient dynamics is a fascinating journey that reveals much about societal values, medical advancements, and human psychology. Over the centuries, this relationship has transformed from one of paternalism to partnership, mirroring broader changes in culture and technology.
In ancient times, the doctor-patient relationship was deeply rooted in mysticism and religion. Physicians were often seen as intermediaries between the divine and the mortal realms. This dynamic was characterized by an implicit trust in the physician's wisdom and authority. Patients rarely questioned their doctors' decisions; instead, they relied on them with a sort of reverential obedience.
As we moved into the Middle Ages, medicine began to incorporate more empirical methods alongside its mystical roots. However, doctors still retained a significant amount of authority over their patients. The concept of "medical paternalism" was prevalent: physicians made decisions on behalf of their patients, believing that they knew what was best for them. This approach assumed that patients lacked the necessary knowledge to make informed choices about their own health.
The Enlightenment era brought significant shifts in thinking across various fields, including medicine. With an emphasis on reason and individual rights, people began to question traditional authorities more openly. In medicine, this led to a gradual shift towards seeing patients as individuals with their own rights and perspectives. However, it wasn't until much later that these ideas fully took root in medical practice.
The 20th century marked a pivotal period in the doctor-patient relationship due primarily to two factors: technological advancements and social change. Medical technologies advanced rapidly during this time-antibiotics, vaccines, imaging technologies-empowering doctors with new tools but also complicating medical decision-making processes. At the same time, movements for civil rights and personal autonomy gained momentum globally.
These societal changes influenced how people viewed authority figures-including doctors-and led to increased demands for patient autonomy in healthcare decisions. By mid-century onwards, there was growing recognition within medical communities worldwide that effective healthcare required collaboration between doctors and patients rather than top-down directives from physicians alone.
This evolving ethos gave rise to concepts such as "informed consent," where patients are provided with comprehensive information about their conditions along with potential treatments so they can make well-informed decisions regarding their care options collaboratively with their healthcare providers.
Today's doctor-patient dynamic is markedly different from its historical counterparts but continues evolving amidst ongoing technological advancements like telemedicine or AI-driven diagnostics systems which alter interactions further still yet emphasize collaborative approaches ensuring better health outcomes overall while respecting individual autonomy simultaneously fostering trust-based relationships built mutual respect shared understanding modern context continually reshaping contours traditional paradigms anew ways reflective contemporary values societal aspirations equitable compassionate care provision all alike irrespective diverse backgrounds circumstances alike thereby enriching humanity collective wellbeing ultimately greater good larger scale
In conclusion then examining historical evolution doctor-patient dynamics provides invaluable insights not only into past practices beliefs shaping current models interaction but also future directions potentially steering field next transformative phase continuing improve enhance quality life countless individuals globally through ever-evolving partnerships grounded mutual trust respect collaboration essential foundations effective compassionate equitable healthcare delivery modern world today tomorrow beyond
Importance of Trust and Communication
The Importance of Trust and Communication in the Doctor-Patient Relationship
In the realm of healthcare, the doctor-patient relationship stands as a cornerstone for effective treatment and patient satisfaction. This bond is built on two pivotal elements: trust and communication. Without these foundational pieces, even the most advanced medical interventions can fall short of achieving optimal outcomes.
Trust serves as the bedrock upon which the doctor-patient relationship is built. When patients trust their doctors, they are more likely to follow prescribed treatments, share vital health information, and feel at ease during consultations. Trust fosters a sense of safety and reassurance; it assures patients that their well-being is in capable hands. In situations involving chronic illnesses or complex treatments, this trust becomes even more critical. It enables patients to navigate uncertainties with confidence, knowing that their physician has their best interests at heart.
Communication acts as the lifeblood that sustains this trust. Effective communication ensures that both parties clearly understand each other's perspectives, concerns, and expectations. For doctors, clear communication involves not only explaining diagnoses and treatment options in understandable terms but also listening actively to their patients' fears and questions. This two-way interaction helps in demystifying medical jargon that often overwhelms patients, making them more informed participants in their own care.
Moreover, good communication extends beyond just verbal exchanges. Non-verbal cues such as eye contact, body language, and facial expressions also play a crucial role in conveying empathy and understanding. When doctors take time to listen attentively and respond thoughtfully, they validate their patients' experiences and emotions. This emotional support can be incredibly healing on its own.
Conversely, poor communication can erode trust rapidly. Misunderstandings about treatment plans or misinterpretation of symptoms can lead to incorrect diagnoses or non-compliance with prescribed therapies. Such breakdowns can cause frustration for both parties involved and may ultimately compromise patient health.
In today's digital age, maintaining open lines of communication has become easier yet more challenging due to technological advancements like telemedicine and electronic health records (EHR). While these tools have facilitated greater access to healthcare services and streamlined information sharing, they also necessitate new skills for effectively communicating through screens rather than face-to-face interactions.
Therefore, continuous efforts must be made to cultivate strong doctor-patient relationships anchored by trust and enriched through effective communication. Medical schools are increasingly recognizing this need by incorporating courses focused on interpersonal skills into their curricula. Likewise, ongoing professional development opportunities for practicing physicians should emphasize these aspects as well.
In conclusion, the importance of trust and communication in the doctor-patient relationship cannot be overstated. These elements not only enhance clinical outcomes but also contribute significantly to patient satisfaction and overall well-being. By prioritizing these values within healthcare practices, we pave the way for more compassionate and effective medical care-one conversation at a time.
Ethical Considerations in the Doctor-Patient Relationship
The doctor-patient relationship is a cornerstone of effective healthcare, and ethical considerations within this dynamic are essential for fostering trust, ensuring patient well-being, and maintaining professional integrity. Ethical considerations in the doctor-patient relationship encompass several key principles: autonomy, beneficence, non-maleficence, and justice.
Autonomy refers to respecting a patient's right to make informed decisions about their own health care. This involves providing patients with all necessary information in a comprehensible manner so they can weigh the benefits and risks of different treatment options. Respecting autonomy means acknowledging that patients have unique values and preferences that must be honored. For instance, some patients may prioritize quality of life over longevity, while others might choose the most aggressive treatments available despite potential side effects.
Beneficence is the principle of acting in the best interests of the patient. This requires doctors to recommend treatments that will benefit the patient while also considering their holistic well-being. The challenge often lies in balancing medical knowledge with individual circumstances-what is medically optimal for one patient may not be for another due to personal or social factors.
Non-maleficence, closely related to beneficence, means "do no harm." Physicians must avoid causing unnecessary harm or suffering through their interventions. This principle underscores the importance of thorough knowledge and skill in medical practice as well as careful consideration when weighing treatment risks against potential benefits.
Justice involves ensuring fairness in medical care delivery. It addresses issues such as equitable access to treatments regardless of socio-economic status, race, gender, or other potentially discriminating factors. In practice, this means advocating for systemic changes that reduce disparities in healthcare access and outcomes.
Confidentiality also plays a critical role in maintaining an ethical doctor-patient relationship. Patients need assurance that their personal health information will be protected unless consent is given otherwise or there's a compelling reason such as risk of harm to others.
Furthermore, informed consent is foundational to ethical interactions between doctors and patients. Patients must be fully informed about their condition and proposed interventions without coercion or undue influence from their healthcare providers.
Finally, empathy and compassion are central to ethical medical practice. These human elements help build rapport and trust between doctors and patients-critical components for effective therapeutic relationships.
In summary, ethical considerations in the doctor-patient relationship are multifaceted but revolve around respecting patient autonomy, practicing beneficence and non-maleficence, ensuring justice and equity in care delivery, maintaining confidentiality, obtaining informed consent appropriately, and approaching each interaction with empathy and compassion. These principles collectively promote a healthcare environment where patients feel valued as individuals with unique needs rather than mere recipients of medical services.
The Role of Technology in Modern Healthcare Interactions
The Role of Technology in Modern Healthcare Interactions: Doctor-Patient Relationship
In the age of rapid technological advancement, the doctor-patient relationship has undergone significant transformation. The integration of technology into healthcare has redefined how doctors and patients interact, offering numerous benefits while also presenting unique challenges. Understanding these dynamics is crucial for fostering a relationship that remains compassionate and effective.
One of the most profound changes brought by technology is the ease of communication between doctors and patients. Telemedicine, for instance, has broken down geographical barriers, allowing patients to consult with specialists from anywhere in the world. This not only increases accessibility to care but also ensures that patients can receive timely medical advice without the need for travel. For individuals in remote or underserved areas, this can be life-changing.
Moreover, electronic health records (EHRs) have streamlined the way information is shared and accessed within the healthcare system. Physicians can now quickly review a patient's medical history, lab results, and treatment plans with just a few clicks. This comprehensive access to data enhances diagnostic accuracy and personalized care. Patients also benefit from having their health information readily available, which empowers them to take an active role in their healthcare decisions.
However, while technology facilitates efficiency and convenience, it can sometimes impede the traditional aspects of doctor-patient interaction that are vital for building trust and empathy. The warmth of face-to-face consultations may be diminished when interactions are conducted through screens or when physicians spend more time inputting data into EHRs than engaging directly with their patients. This shift necessitates a balance where technology supports rather than overshadows human connection.
Another notable development is the rise of wearable health devices and mobile applications that monitor various health parameters such as heart rate, blood sugar levels, and physical activity. These tools provide real-time data that can help doctors make informed decisions about treatment plans while enabling patients to track their progress more closely. Yet, this constant flow of information can be overwhelming for both parties if not managed properly.
The digital divide also poses a challenge; not all patients have equal access to technological resources or possess the digital literacy needed to navigate them effectively. Ensuring inclusivity means providing alternative options for those who might be left behind by tech-driven healthcare models.
Despite these challenges, there are promising ways forward. Training programs focusing on communication skills alongside technical proficiency can help healthcare professionals maintain empathy while utilizing new technologies. Moreover, integrating patient feedback into the design and implementation of technological tools ensures they meet real-world needs without diminishing personal interaction.
In conclusion, technology plays an indispensable role in modern healthcare interactions by enhancing accessibility, efficiency, and patient empowerment within the doctor-patient relationship. However, it is imperative that we remain vigilant about preserving the human elements of care-compassionate listening, empathy, and personal connection-that form the bedrock of effective medical practice. By striking a harmonious balance between innovation and humanity, we can ensure that technology serves as an ally rather than an obstacle in our journey towards better health outcomes.
Impact of Cultural and Social Factors on Doctor-Patient Relations
The Impact of Cultural and Social Factors on Doctor-Patient Relations
In the intricate dance of healthcare, the relationship between a doctor and their patient is paramount. This connection often determines the quality of care, patient satisfaction, and health outcomes. However, this relationship doesn't exist in a vacuum; it is deeply influenced by cultural and social factors that both parties bring to the table.
Cultural factors shape our beliefs, values, and behaviors from a young age. They determine how we perceive illness, wellness, and medical intervention. For instance, in some cultures, mental health issues may be stigmatized or viewed as a personal weakness rather than a medical condition requiring treatment. This can lead to patients either avoiding seeking help altogether or withholding critical information from their doctors out of fear or shame. On the other hand, there are cultures where traditional medicine holds significant sway. Patients from such backgrounds might be skeptical of modern medical practices or prefer natural remedies over prescribed medications.
Language barriers present another significant cultural hurdle in doctor-patient relations. Effective communication is the cornerstone of any relationship, more so in healthcare where clear understanding can mean the difference between life and death. When patients and doctors do not share a common language, misdiagnoses become more likely due to misunderstandings or incomplete information gathering. Even when interpreters are available, nuances can get lost in translation, leading to less effective care.
Social factors also play a crucial role in shaping doctor-patient interactions. Socioeconomic status can affect access to healthcare services and influence perceptions about the quality of care received. Patients from lower socioeconomic backgrounds might face challenges such as lack of insurance coverage or transportation issues that hinder their ability to attend appointments regularly. These barriers create stress and may foster feelings of distrust towards healthcare providers who they feel do not understand their struggles.
Moreover, education levels impact health literacy-patients' ability to obtain, process, and understand basic health information needed to make informed decisions about their health. Lower health literacy can lead to poor management of chronic conditions and lower adherence to treatment plans because patients might not fully grasp the importance or instructions provided by their doctors.
Furthermore, social determinants like race and ethnicity cannot be overlooked when discussing doctor-patient relationships. Studies have shown that minorities often receive different levels of care compared to their white counterparts due to implicit biases held by some healthcare providers. These biases can manifest in various ways-ranging from dismissive attitudes towards pain complaints to assumptions about lifestyle choices-that ultimately compromise the quality of care delivered.
To navigate these complex cultural and social landscapes effectively requires sensitivity and adaptability on part of both doctors and patients. Medical professionals need ongoing training in cultural competence-an awareness of one's own cultural worldview alongside an open-mindedness towards others' worldviews-to bridge gaps created by cultural differences genuinely successfully.
Patients also benefit from being proactive participants in their healthcare journey: asking questions when unsure about something related directly impacting them medically speaking while communicating openly regarding traditional beliefs potentially affecting prescribed treatments' effectiveness (or perceived efficacy).
In conclusion: The interplay between culture/social dynamics significantly shapes how doctors connect with those they serve; recognizing/addressing these influences head-on fosters stronger bonds vital improving overall outcomes within our ever-diversifying global population contexts today!
Challenges and Solutions in Maintaining Healthy Relationships
The doctor-patient relationship is a cornerstone of effective healthcare, but maintaining a healthy and productive interaction between doctors and patients is not without its challenges. These obstacles can stem from communication barriers, time constraints, differing expectations, and emotional complexities. However, by understanding these challenges and employing thoughtful solutions, we can foster stronger relationships that ultimately enhance patient care.
One of the primary challenges in the doctor-patient relationship is communication. Misunderstandings can arise due to medical jargon that patients may not understand or cultural differences that affect how information is perceived. To address this issue, doctors should strive to use clear, simple language when explaining diagnoses and treatments. Additionally, active listening skills are essential; doctors must give patients the opportunity to express their concerns fully before jumping to conclusions or recommendations.
Time constraints also pose a significant challenge. In many healthcare settings, doctors are under pressure to see a high volume of patients within limited time frames. This rush can lead to incomplete assessments and make patients feel unheard or undervalued. One solution involves optimizing appointment schedules to allow for longer consultations where necessary. Moreover, implementing efficient electronic health record systems can help streamline administrative tasks, giving doctors more time for meaningful patient interactions.
Differing expectations between doctors and patients can further complicate this relationship. Patients may come in with preconceived notions about their conditions or treatment plans based on internet research or anecdotal advice from friends and family. On the other hand, doctors might approach cases based on clinical guidelines that do not always align with individual patient preferences or lifestyles. Bridging this gap requires open dialogue where both parties discuss their views candidly. Shared decision-making models encourage collaboration and ensure that treatment plans reflect both medical expertise and patient values.
Emotional complexities also play a role in challenging doctor-patient relationships. Chronic illnesses or severe diagnoses often bring about strong emotions such as fear, anger, or sadness which can affect communication dynamics negatively. Doctors need to recognize these emotional states and respond with empathy rather than dismissiveness. Training in emotional intelligence can equip healthcare providers with the skills needed to navigate these sensitive situations effectively.
Furthermore, trust forms the bedrock of any healthy doctor-patient relationship but building it demands consistent effort over time. Transparency about treatment options including risks involved helps cultivate trustworthiness among patients while confidentiality assures them about safety regarding personal information shared during consultations.
In conclusion though maintaining healthy relationships between doctors & patients presents several challenges ranging from communication barriers & time constraints through differing expectations up until dealing with complex emotional states yet each obstacle comes along potential solutions rooted mainly around improved communication practices empathetic approaches flexible scheduling enhanced cooperation via shared decision-making models alongside consistent efforts towards establishing mutual trust thereby ensuring better overall healthcare outcomes fostering greater satisfaction levels amongst both parties involved
Future Trends and Perspectives
The doctor-patient relationship has long been the cornerstone of effective healthcare. As we progress further into the 21st century, this dynamic is set to undergo significant transformations driven by technological advancements, evolving societal norms, and changes in healthcare delivery models. Understanding these future trends and perspectives is critical for both medical professionals and patients alike.
One of the most prominent trends shaping the future of the doctor-patient relationship is the integration of digital health technologies. Telemedicine, once a niche practice, has now become mainstream thanks to advancements in communication technologies and a global pandemic that necessitated remote consultations. This shift allows patients to access care from the comfort of their homes, making healthcare more accessible than ever before. However, it also poses challenges in maintaining personal connections that are often vital for effective care. Moving forward, striking a balance between convenience and personal touch will be crucial.
Artificial Intelligence (AI) is another game-changer poised to redefine how doctors interact with their patients. AI can assist in diagnosing conditions, predicting patient outcomes, and personalizing treatment plans based on vast amounts of data that go beyond human capability to process comprehensively. While this promises improved accuracy and efficiency in medical care, it also raises questions about trust and accountability. Patients may find themselves needing reassurance about the role of AI in their treatment plans and whether it might override or complement human judgment.
As society becomes increasingly aware of mental health issues, there is a growing emphasis on holistic approaches that consider both physical and psychological well-being. Future doctor-patient relationships will likely see more integrated care teams comprising not just physicians but also mental health professionals, nutritionists, and social workers working collaboratively. This multidisciplinary approach aims to treat patients as whole individuals rather than just addressing isolated symptoms or conditions.
Moreover, patient empowerment is expected to play a more significant role in future healthcare interactions. With easy access to medical information online and tools that monitor health metrics at home, patients are becoming more knowledgeable about their conditions and potential treatments. This shift necessitates a transformation from paternalistic models of care towards partnerships where doctors act as advisors guiding informed decision-making processes rather than dictating them.
Data privacy remains an ongoing concern as digital records become ubiquitous in managing patient information. Ensuring robust security measures while maintaining ease of access for authorized personnel will be an ongoing balancing act. Trust will be fundamental here; patients need assurance that their sensitive information is secure yet available when necessary for their treatment.
Lastly, cultural competence will continue to gain importance in doctor-patient relationships as societies become more diverse globally. Healthcare providers must be adept at navigating different cultural norms and values to provide equitable care effectively.
In conclusion, while technology offers numerous opportunities for enhancing healthcare delivery through improved accessibility, personalized treatment plans using AI insights or telehealth services - it simultaneously presents challenges like ensuring data privacy or maintaining personal connections amidst digital interactions which require thoughtful navigation moving forward alongside greater emphasis on holistic approaches considering both physical & psychological well-being together within culturally competent frameworks ultimately fostering stronger partnerships between empowered patients & advisory-role physicians alike thereby enhancing overall quality-of-life outcomes sustainably over time!